Stroke Management in 2022: Part 2
Alex Rowell, Fahad Ashraf, Greg Selkirk & Luke Torre continue their discussion stroke management. In this talk they tackle imaging and treatment of stroke, including mechanical thrombectomy.
Imaging is an enormous part of the process of stroke management. It is critical for diagnosis and stratifying patient treatments.
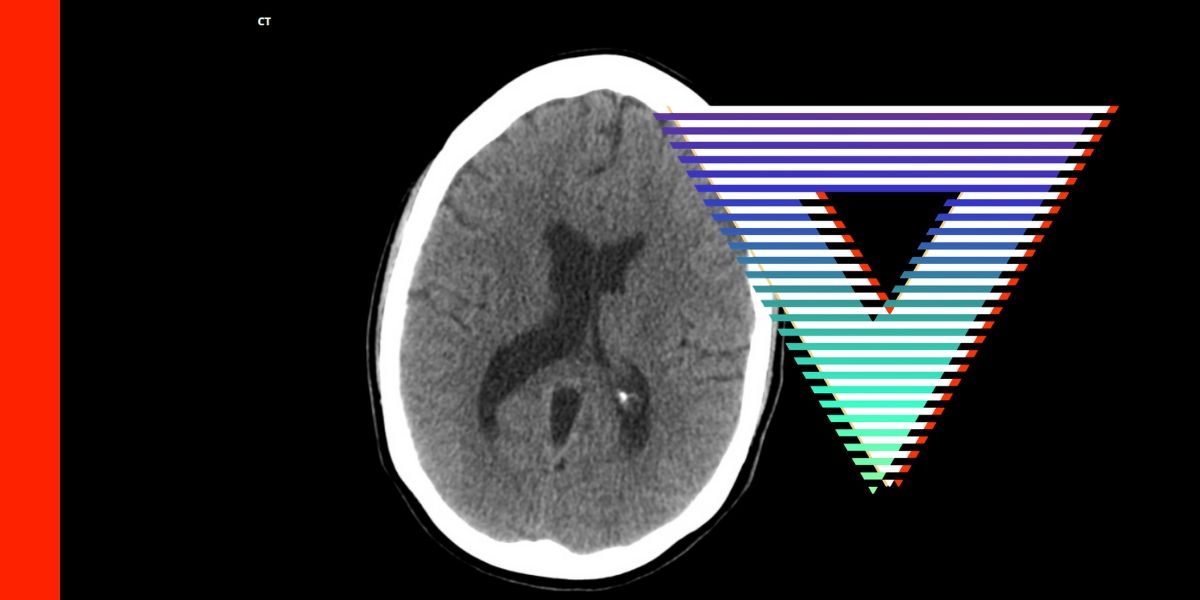
The first imaging modality to order is a non-contrast CT head. As Greg explains, not everyone with neurological symptoms has an ischemic stroke. Other diagnoses to consider include Todd’s paresis and intracranial haemorrhage. The CT will also inform the clinician how much established infarct is present and give an indication of where the clot is.
Moreover, carotid angiogram should be used to assess the intracranial vessels. It also allows one to plan the fastest way to remove a clot, should it be present. Transradial and transfemoral thrombectomy are two options. The imaging provides the clinician with valuable information about the most efficient and fastest way of reaching the clot for removal.
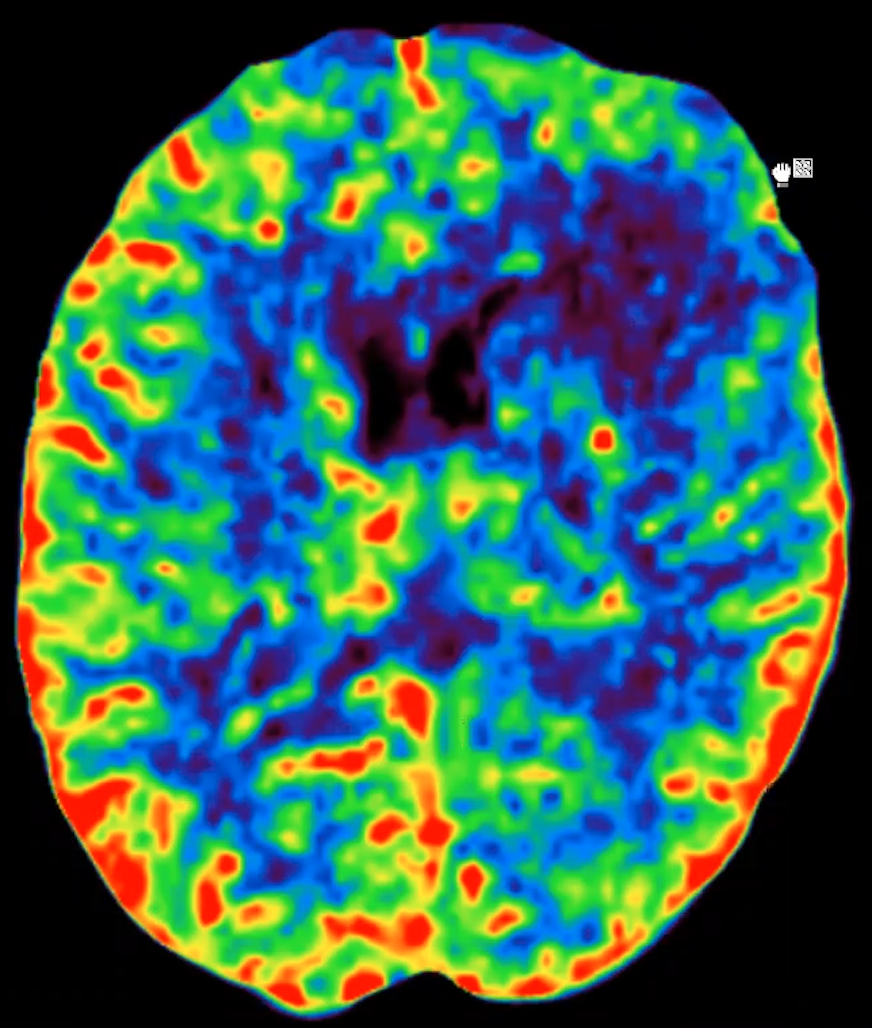
Lastly, the team discuss CT perfusion. A word of warning. This exists as a problem-solving test. It is a good idea to interpret with caution!
Evidently, geographical location and the availability of imaging resources restricts imaging.
Where CT scanning is available, this modality combined with a thorough history and assessment of deficits can lead the clinician towards the most appropriate treatment options – including thrombolysis.
The question then becomes, does the use of thrombolysis in a rural or remote location preclude the eventual use of thrombectomy? As Greg explains, thrombolysis works well in conjunction with thrombectomy. Receiving thrombolysis does not preclude the use of thrombectomy and does offer advantages.
Furthermore, Greg will provide a detailed description on the procedure of thrombectomy, including the various methods used and the care of the patient after a thrombectomy. He touches on the use of general anaesthesia during the procedure, as well as antiplatelet therapy post-intervention.
Thrombectomies are not without risks. Complications include perforation of blood vessels. From a neurological perspective, Fahad describes the use of repeat scanning to ensure the absence of any subsequent bleeding and the implications for ongoing medical therapy.
Finally, the discussion concludes with a broader take on stroke services in general. This includes pre-hospital stroke awareness in the community, post stroke rehabilitation and neuroprotection measures.
For more head to our podcast page #CodaPodcast
Please see below for images referred to in the talk.

Left M1 cerebral artery:
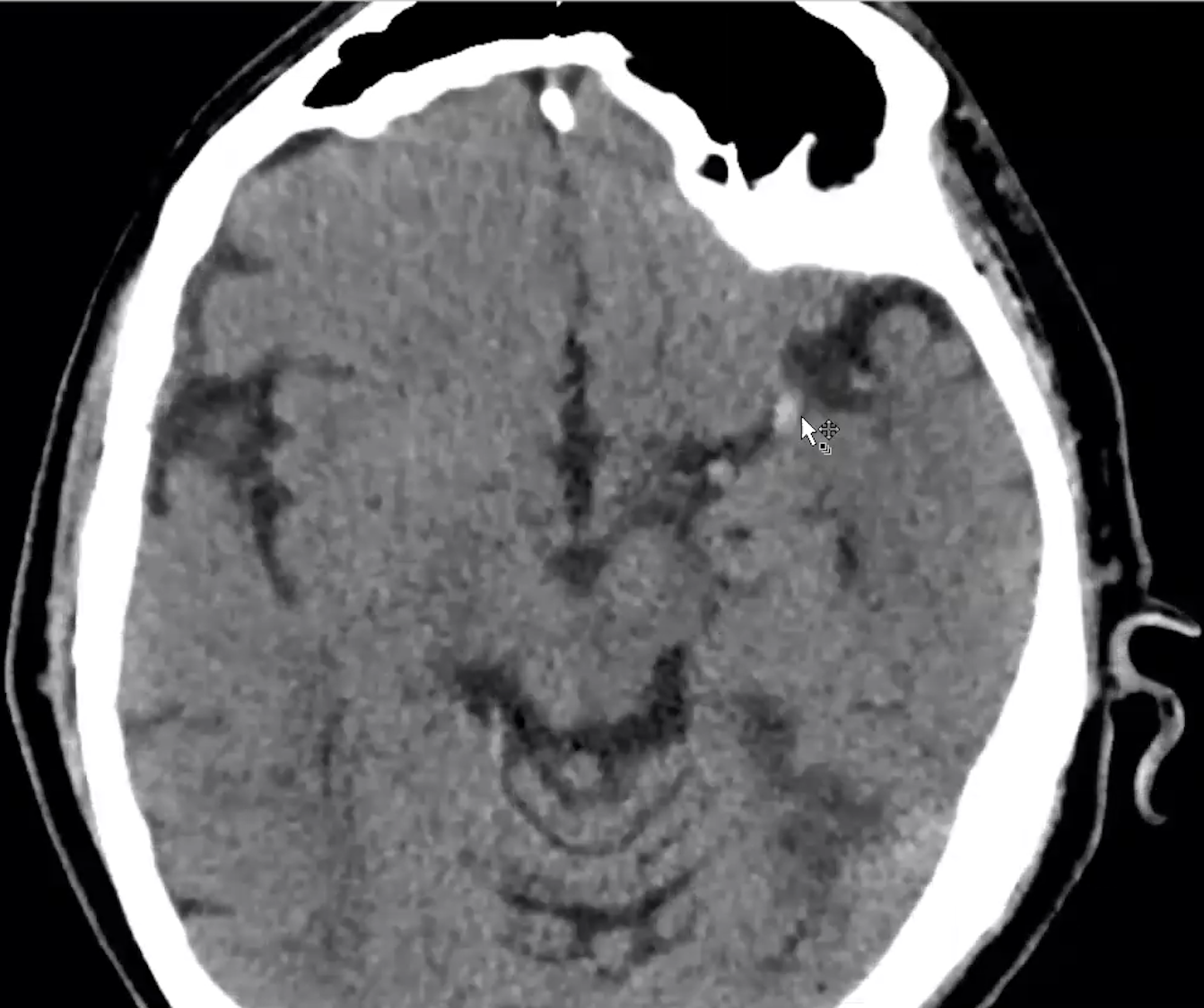
Grey white matter is maintained:
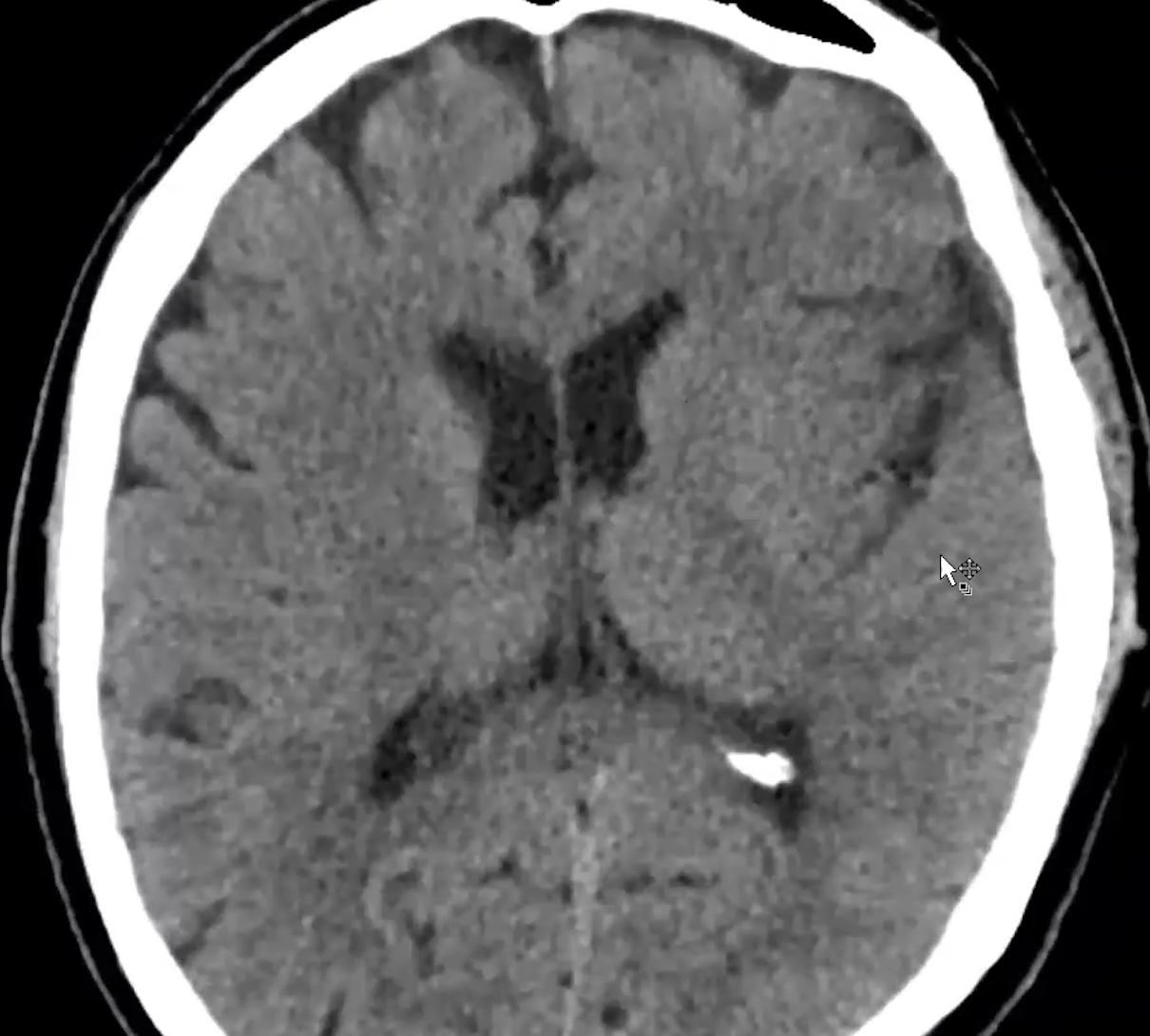
Terminal ICA:
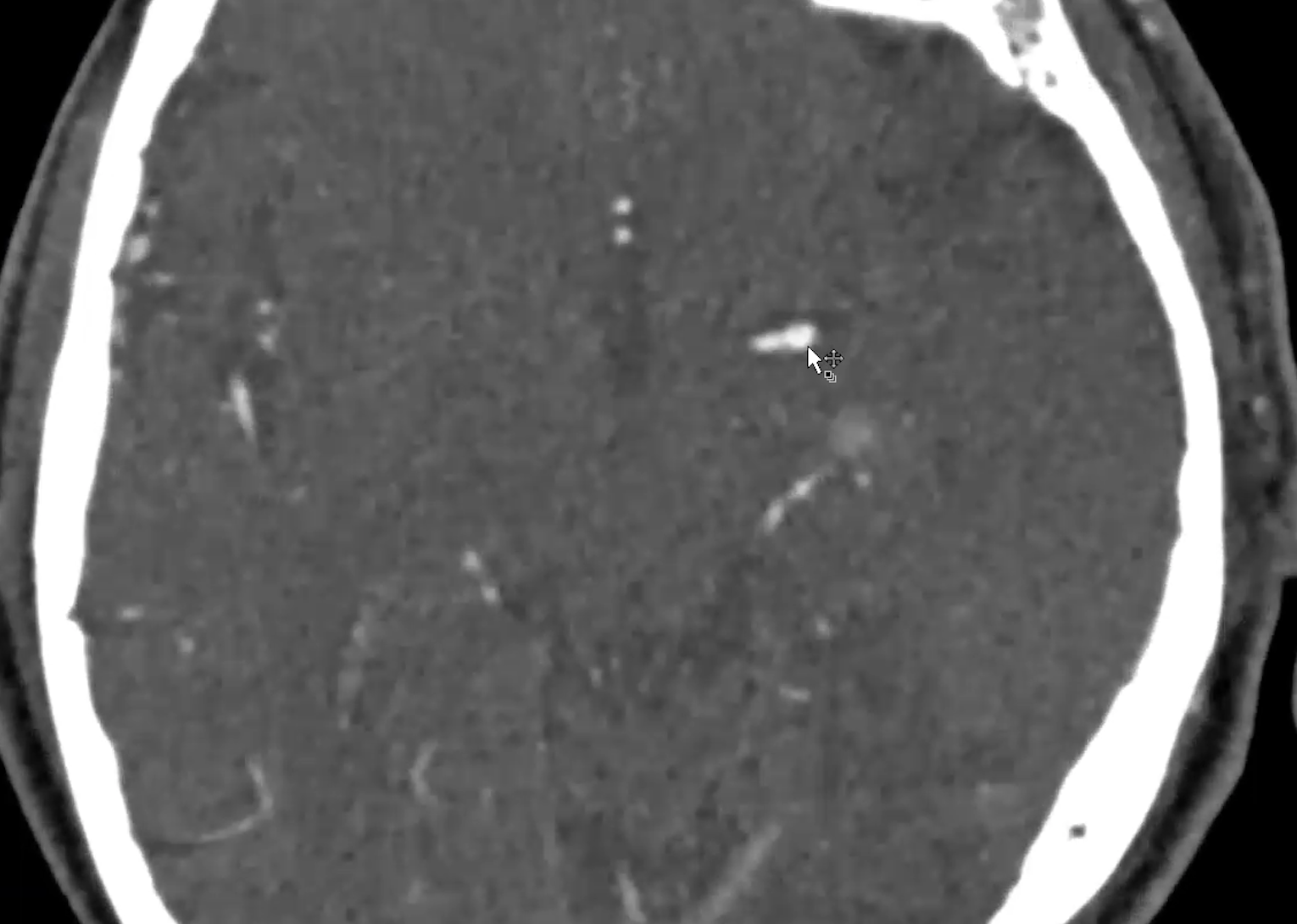
Right A1 cuts off abruptly:
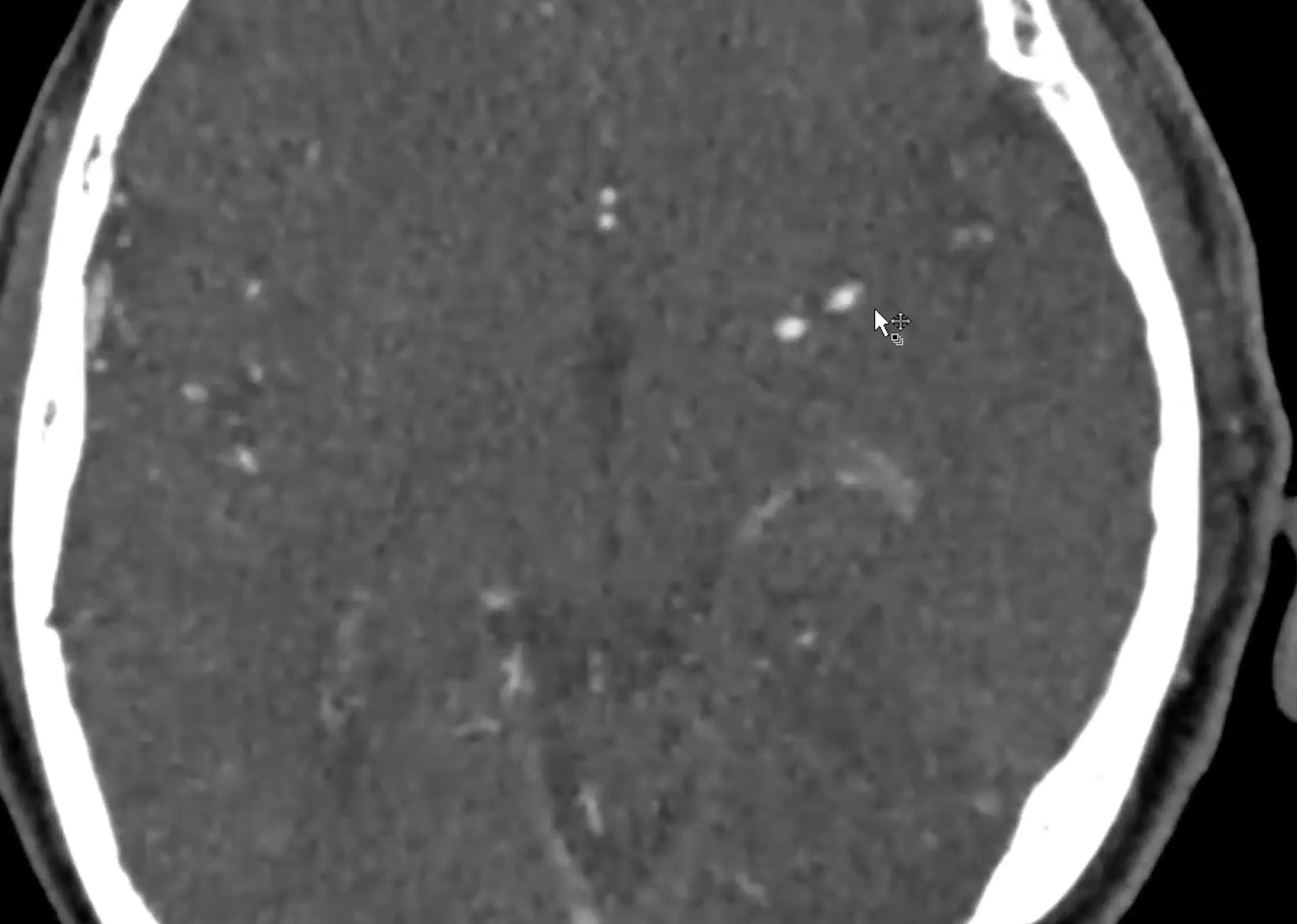
Cerebral blood flow is markedly impaired:
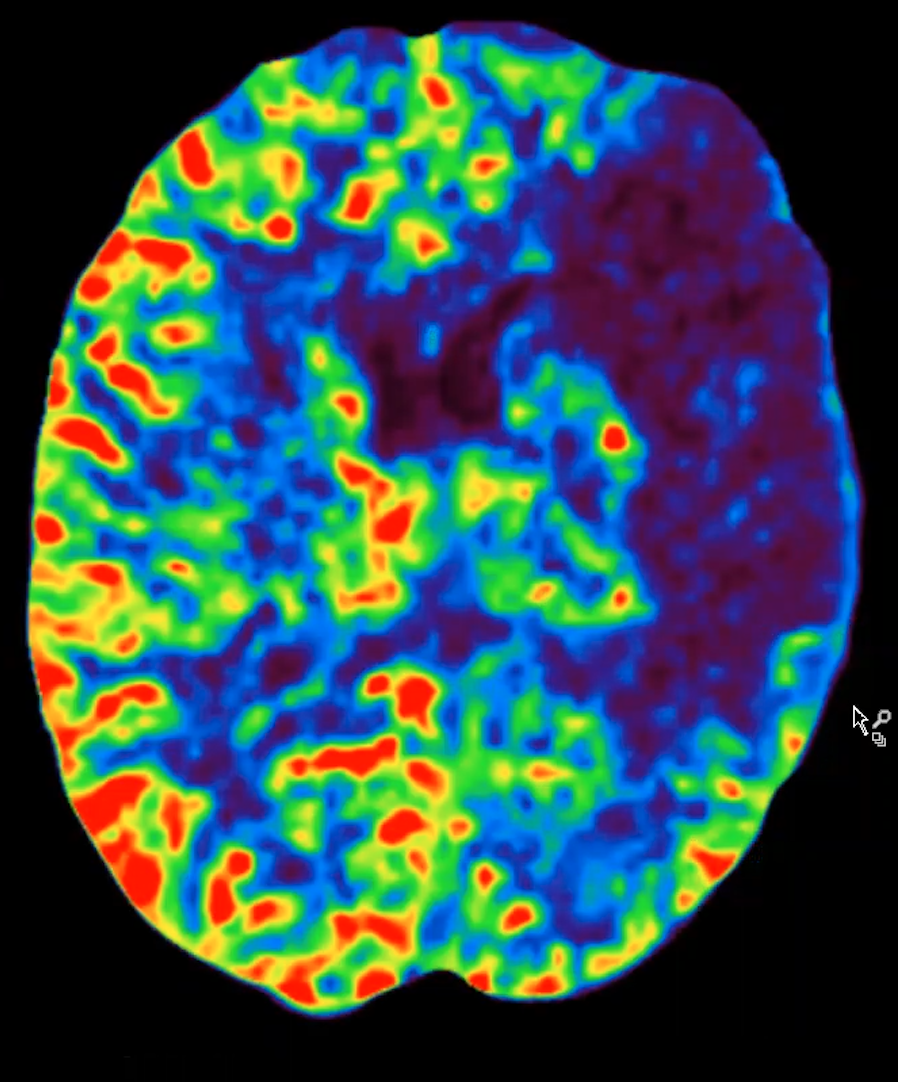
Cerebral blood volume: